Looking for a Superbill Template to help with your insurance claims? Read this guide to learn what you need to know about superbills and download our free template to streamline your billing process. Whether you’re managing out-of-network claims or running a private practice, this guide walks you through how to fill out, store, and use a superbill effectively to support accurate, compliant reimbursement.
## **What is a superbill?**
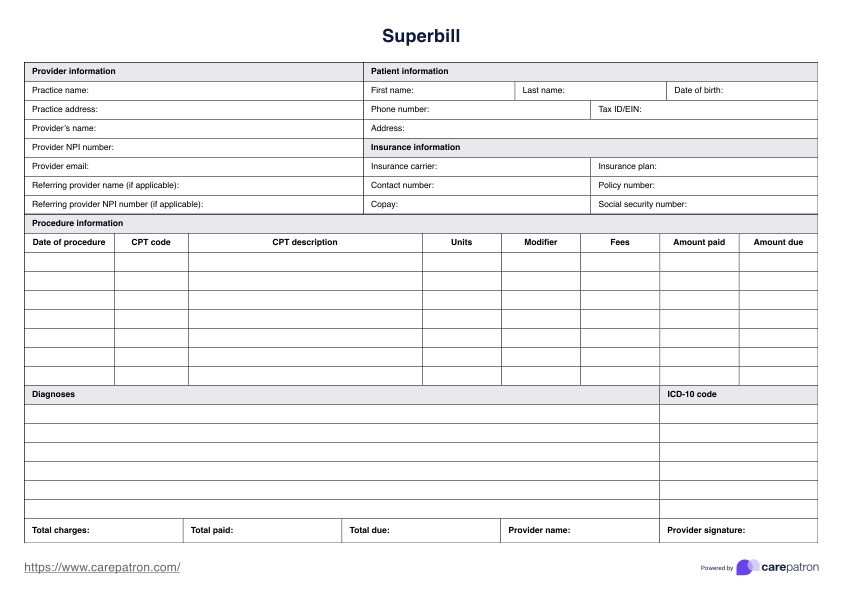
A superbill is a detailed document that healthcare providers use to summarize the services delivered to a patient for insurance reimbursement. It serves as a bridge between clinical care and the medical billing process, containing all the information needed for claims submission to an insurance provider. A superbill typically includes patient and provider details, the insurance plan, CPT and ICD-10 codes, dates of service, and associated charges. As the main record for claims sent to payers—especially for out-of-network services—it’s vital for ensuring accurate and timely reimbursement. Properly completed superbills are key to compliant billing and reducing claim rejections.
Using a superbill helps standardize coding systems and billing processes, reducing documentation errors and saving time with a ready-to-fill structure. It also improves data accuracy and security through digital completion and encrypted storage. Dedicated spaces for [CPT codes](https://www.carepatron.com/procedure-code/) and [ICD-10 codes](https://www.carepatron.com/icd/) ensure clarity, while sections for total charges and payments make reimbursement tracking easier for both providers and patients.
However, because superbills are completed manually, there’s still a risk of human error or duplication when entering data into payer portals. They may also be less practical for large, high-volume organizations.
## **How to use our free Superbill Template**
Our Superbill Template can be used to create an itemized list of the services your patient received. As this superbill is the primary information source for your patient's medical insurance claim, it's very important that the information it contains is accurate and meets the information requirements of the insurance company or payer. To help prevent your client's claim from being rejected, just follow these steps.
### **Step 1: Provider, insurance and patient information**
Fill out each of these sections with the relevant information, being sure to include the provider NPI, patient date of birth and address, and your patient's insurance details.
### **Step 2: Procedures**
The procedure information section is for the list of services rendered and procedures your patient received from your practice. For the sorts of procedures included in this section, take a look at the most commonly used CPT codes (also called procedure codes). Ensure you add the relevant CPT code for the procedure, any modifiers, as well as the units, fees, and payment information.
### **Step 3: Diagnoses**
Similar to procedures, diagnoses must also be accompanied by ICD-10 diagnosis codes. It's important to be clear on the difference between ICD and CPT codes, as errors in medical coding can result in rejected claims.
### **Step 4: Payment totals**
To make the total payment due crystal clear, we have included space for the total charges, total paid, and Total Due at the bottom of the Superbill Template. You can calculate these figures using the fees, amount paid, and amount due columns in the procedure information section.
### **Step 5: Sign the superbill and securely store a copy**
The final step is for the provider to sign the superbill, return a copy to either the patient or directly to the insurance company, and store a copy securely for record-keeping purposes.
## **Common mistakes to avoid when completing a superbill**
Even small errors on a superbill can cause claim delays, denials, or compliance issues. Because superbills serve as the primary documentation for insurance reimbursement, accuracy and completeness are essential. Here are some of the most common mistakes healthcare providers make when completing a superbill—and how to avoid them:
### **Missing or incorrect CPT and ICD-10 codes**
One of the most common and costly mistakes is entering the wrong CPT or ICD-10 code, or leaving them out altogether. Each service provided must correspond with the correct diagnosis and procedure codes. When codes are mismatched or outdated, payers may deny the claim or require resubmission. To prevent this, always use the most current coding sets from the American Medical Association and Centers for Medicare & Medicaid Services and verify that codes align with the documentation in the patient’s chart.
### **Omitting provider or patient information**
Claims can also be rejected when key identifying details are missing. Common omissions include the provider’s National Provider Identifier (NPI), patient’s date of birth, or insurance policy number. The CMS Medicare Claims Processing Manual (n.d.) notes that incomplete information is one of the top reasons for rejected or returned claims. Using a structured template like Carepatron’s ensures that every required field—both clinical and administrative—is filled out before submission.
### **Failing to include modifiers**
Modifiers clarify the circumstances of care, such as when a procedure was repeated, adjusted, or performed bilaterally. Forgetting or misusing modifiers can result in underpayment or claim rejection. Modifiers must accurately reflect how the procedure was performed to avoid billing discrepancies. Always review whether modifiers apply before submitting the superbill.
### **Miscalculating totals or leaving charges incomplete**
Mathematical or clerical errors in charge totals can cause inconsistencies between the superbill and the claim submission. These discrepancies often trigger payer reviews or payment delays. It’s best practice to review the “total charges,” “total paid,” and “total due” fields carefully and ensure they match the procedure information above.
### **Not storing superbills securely**
Superbills contain sensitive patient health and billing data, which means they must be protected in line with HIPAA regulations. The U.S. Department of Health and Human Services (2025) advises that all documents containing protected health information (PHI) should be encrypted or stored in a secure, access-controlled environment. Using [HIPAA-compliant software](https://www.carepatron.com/templates/hipaa-compliant-software/) like Carepatron makes it easier to store and retrieve superbills safely without risking data breaches.
## **References**
Centers for Medicare & Medicaid Services. (n.d.). Medicare Claims Processing Manual (Publication 100-04). U.S. Department of Health and Human Services. Retrieved October 20, 2025, from https://www.cms.gov/medicare/regulations-guidance/manuals/internet-only-manuals-ioms
U.S. Department of Health and Human Services. (2025, March 14). Summary of the HIPAA privacy rule. https://www.hhs.gov/hipaa/for-professionals/privacy/laws-regulations/index.html