Looking for a tool that can measure how patients feel about their osteoarthritis? Read our guide to learn about the WOMAC Osteoarthritis Index, then download our template so you can use it to measure the effect of osteoarthritis on your patient.
## **An overview of osteoarthritis**
Osteoarthritis (OA) is the most common form of arthritis, a chronic condition where the protective cartilage that cushions the ends of bones in a joint wears down over time. This degeneration means the cartilage loses its elasticity and can eventually wear away entirely, leading to bones rubbing against each other. It emerges largely from this "wear and tear" process, accelerated by factors like older age, obesity, previous joint injury, genetics, and repetitive stress on the joints. Though any joint can be affected, OA is most common in the knees, hips, hands, and spine (Mayo Clinic, 2025).
The main symptoms of OA are joint pain that often worsens with activity and improves with rest, and stiffness, particularly after waking up or sitting still. Other common symptoms include a limited range of motion, tenderness, swelling, and a grating, crackling, or popping sound/sensation (crepitus) when moving the joint (Whelan, 2018).
The problems OA can cause extend beyond joint discomfort; they include significant limitations in daily activities like walking or climbing stairs, difficulty sleeping due to pain, and a higher risk of complications such as falls, muscle weakness, and mental health issues like anxiety and depression due to chronic pain and reduced mobility (Healthdirect, 2024). While OA damage cannot be reversed, treatments aim to manage symptoms and improve function.
## **What is the WOMAC Osteoarthritis Index?**
The Western Ontario and McMaster Universities Osteoarthritis Index, or WOMAC Osteoarthritis Index for short, is one of healthcare professionals' most valuable assessment tools to assess hip and knee (OA) osteoarthritis as well as back pain, rheumatoid arthritis, and fibromyalgia. It is a 24-item list. Professionals hand it out to patients with hip or knee osteoarthritis and have them rate themselves per item.
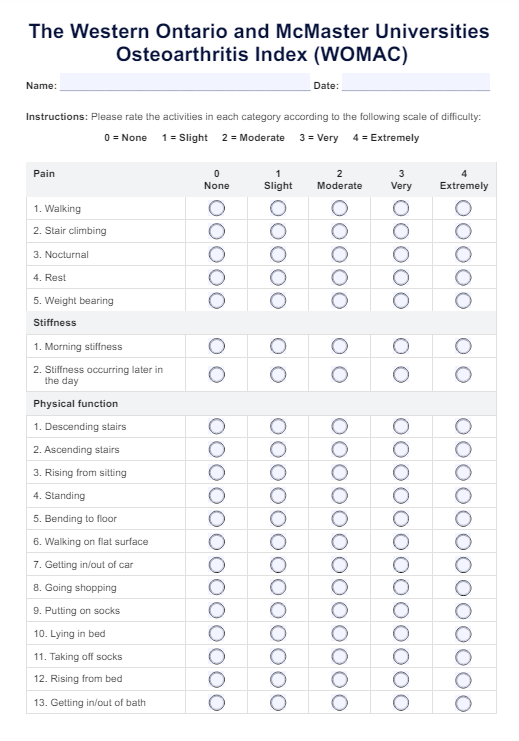
The 24 items on the WOMAC index are divided into three sections:
- WOMAC pain subscale (five items)
- WOMAC stiffness subscale (two items)
- WOMAC physical function subscale (seventeen items)
These subscales and items revolve around the functional limitations of patients with knee osteoarthritis or hip osteoarthritis and how either one or both affect their activities of daily living, quality of life, and general health and well-being.
### **How is it scored?**
Patients answering the WOMAC index will rate themselves for each subscale based on the difficulty caused by their osteoarthritis. Each item can be rated from 0 to 4:
- 0 = None
- 1 = Slight
- 2 = Moderate
- 3 = Very
- 4 = Extremely
Patients are only allowed to pick one number rating per item.
Once the patient has rated all items, they must submit the report back to the healthcare professional who gave it to them, and then the professional will start calculating the scores.
The healthcare professionals only need to get the sum for each subscale and the total osteoarthritis outcome score.
They must divide the total score by 96 to calculate the final score. 96 is the maximum possible score (if patients rated themselves 4 for all 24 items). The total score indicates the percentage of difficulty osteoarthritis causes in the patient.
### **Reliability and limitations**
The Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) is considered a reliable and valid patient-reported outcome measure for assessing pain, stiffness, and physical function in patients with knee and hip osteoarthritis (Roos et al., 1999). It is one of the most widely used and recommended outcome measures for OA clinical trials and practice, with numerous validation studies across different cultures and languages confirming its strong psychometric properties, including high internal consistency and satisfactory test-retest reliability across its subscales (Zhao et al., 2025).
Aside from the reliability of the WOMAC, one of the great things about self-report outcome measures such as the WOMAC index is that they provide healthcare professionals with their patients' perspectives. While professionals can make objective assessments of osteoarthritis, it's also important to know how exactly the patient feels about their ailment and the difficulties they face as a result. Knowing the patient's side of things can help professionals determine the best and most personalized treatment that suits their patient's needs.
However, the WOMAC index has a few notable limitations. One significant issue is the variability and inconsistency in how it's used and reported across clinical trials, particularly regarding the specific scale and scoring range, which can lead to ambiguity and difficulty in interpreting and comparing results between studies (Woolacott et al., 2012). A deeper limitation is the potential inability to completely distinguish between changes in pain and changes in function (Stratford et al., 2018), which could lead a clinician to form an inaccurate impression of a patient's mobility status, especially when assessing therapeutic response.
### **Next steps after using this index**
The next steps might vary depending on the final score and percentage calculated by the healthcare professional. Conservative treatments might be the best option if the difficulty is low or moderate. These include taking medications like non-steroidal anti-inflammatory drugs (NSAIDs) and acetaminophen. Taking physical and occupational therapy can help restore strength in the hip or knee and find ways to lessen the stress on those joints.
For those with higher final scores and percentages, such as in the WOMAC function subscale, further testing should be conducted to determine if it would be best for patients to take cortisone/lubrication injections or undergo surgery (hip joint replacement, total knee replacement, or bone realignments). As with all surgeries, risks must be assessed and relayed to patients to help them decide on the treatment they need.
## **How to use our WOMAC Osteoarthritis Index template**
Conducting the WOMAC Osteoarthritis Index is typically a self-administration process for the patient, overseen by a clinician or researcher who provides the initial instructions. The index is generally divided into three sections: Pain, Stiffness, and Physical Function. Here is a short, step-by-step guide based on common administration practices for the Likert scale version:
### **Step 1: Preparation and explanation**
Provide the patient with a copy of the questionnaire and a writing instrument (pen/pencil). Then, explain that the questionnaire assesses pain, stiffness, and difficulty with daily activities over the last 48 hours (or another specified time frame, like the last week, depending on the version used).
Don't forget to clarify that the patient should answer EVERY question with only ONE response from the available options.
### **Step 2: Answer section A**
Instruct the patient to rate the amount of pain they experienced in the affected joint (hip or knee) for each of the five listed activities (e.g., walking, sleeping, standing). The rating scale is typically 0 (None) to 4 (Extreme).
### **Step 3: Answer section B**
Instruct the patient to rate the severity of stiffness they experienced, not pain, for the two listed times (e.g., morning stiffness, stiffness after resting). Use the same 0 (None) to 4 (Extreme) rating scale.
### **Step 4: Answer section C**
Instruct the patient to indicate the degree of difficulty experienced with 17 specific physical activities (e.g., descending stairs, rising from a chair, putting on socks). Use the 0 (None) to 4 (Extreme) rating scale for difficulty.
### **Step 5: Scoring and finalization**
Once the patient is finished answering, calculate the subscale scores by summing the circled numbers for each section. Afterward, calculate the Total WOMAC Score by adding the three subscale scores.
As an optional step, normalize the raw scores to a 0–100 scale by multiplying the subscale or total raw score by a factor to represent a percentage, where a higher score indicates worse function/more pain
## **Additional resources**
Looking for additional resources to supplement the WOMAC Osteoarthritis Index?
- **[Osteoarthritis Diagnosis Criteria](https://www.carepatron.com/templates/osteoarthritis-diagnosis-criteria/#app-chapter-four)**: Identify osteoarthritis early on or enhance the accuracy and consistency of your osteoarthritis diagnosis with our template, where you can record your findings.
- **[Knee Injury and Osteoarthritis Outcome Score (KOOS)](https://www.carepatron.com/templates/koos/#app-chapter-one)**: Assess short-term and long-term symptoms and functions in individuals experiencing various types of knee pain/injuries and osteoarthritis.
- **[Activities of Daily Living Checklist](https://www.carepatron.com/templates/activities-of-daily-living/)**: Track your patient's level of independence to formulate a better care or treatment plan.
## **References**
Healthdirect. (2024). Osteoarthritis. https://www.healthdirect.gov.au/osteoarthritis#:~:text=poor%20sleep%20due%20to%20pain,it%20is%20affecting%20your%20life.&text=Your%20doctor%20may%20refer%20you,you%20manage%20your%20daily%20activities.
Mayo Clinic. (2025). Osteoarthritis. https://www.mayoclinic.org/diseases-conditions/osteoarthritis/symptoms-causes/syc-20351925
Roos, E. M., M. Klässbo, & Lohmander, L. S. (1999). WOMAC Osteoarthritis Index: Reliability, validity, and responsiveness in patients with arthroscopically assessed osteoarthritis. Scandinavian Journal of Rheumatology, 28(4), 210–215. https://doi.org/10.1080/03009749950155562
Stratford, P., Kennedy, D., & Clarke, H. (2018). Confounding pain and function: the WOMAC’s failure to accurately predict lower extremity function. Arthroplasty Today, 4(4), 488–492. https://doi.org/10.1016/j.artd.2018.09.003
Whelan, C. (2018, January 9). Everything You Need to Know About Osteoarthritis. Healthline; Healthline Media. https://www.healthline.com/health/osteoarthritis
Woolacott, N. F., Corbett, M. S., & Stephen. (2012). The use and reporting of WOMAC in the assessment of the benefit of physical therapies for the pain of osteoarthritis of the knee: findings from a systematic review of clinical trials. Lara D. Veeken, 51(8), 1440–1446. https://doi.org/10.1093/rheumatology/kes043
Zhao, Y., Zhang, Y., Liu, K., Chai, Y., Yan, H., Lin, F., Zhan, H., Zheng, Y., & Yuan, W. (2025). Test the reliability and comparability of the paper version and electronic version of the Western Ontario and McMaster University Osteoarthritis Index in Chinese language: a randomized, cross-sectional study. Clinical Rheumatology, 44(10), 4325–4334. https://doi.org/10.1007/s10067-025-07572-z